

|
What They Are, How They Work,
When to Use
Them
By Martin Markowitz, MD
Dr. Markowitz is a Staff Investigator at the Aaron
Diamond AIDS
Research Center and Assistant Professor of Medicine at New York
University School
of Medicine in New York City.
Revised and published by IAPAC July, 1996
![]() Introduction
Introduction![]() 1. What are HIV
infection and
AIDS?
1. What are HIV
infection and
AIDS?![]() 2. What is HIV
protease?
2. What is HIV
protease?![]() 3. What are protease inhibitors and how do
they work?
3. What are protease inhibitors and how do
they work?![]() 4. Will protease inhibitors get rid of HIV?
4. Will protease inhibitors get rid of HIV?![]() 5. How do protease inhibitors differ from other
5. How do protease inhibitors differ from other
available anti-HIV drugs?![]() 6. What protease inhibitors are being studied
now?
6. What protease inhibitors are being studied
now?![]() 7. Can protease inhibitors be combined with
other
drugs?
7. Can protease inhibitors be combined with
other
drugs?![]() 8. Can protease inhibitors be combined with
each
other?
8. Can protease inhibitors be combined with
each
other?![]() 9. What side effects do protease inhibitors have
9. What side effects do protease inhibitors have
by themselves?![]() 10. What is resistance and how big of a
problem is
it?
10. What is resistance and how big of a
problem is
it?
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
Introduction
Words printed in italics the first time they appear are linked to explanations in the Word List page. Click on the word on the Word List page, and you'll be returned to the words place on this page.
Protease inhibitors are drugs that slow down the spread of HIV--the virus that causes AIDS inside the body. Using measurements of HIV circulating in the blood, studies of protease inhibitors in people with HIV show that these drugs are more powerful than the first group of drugs used to treat HIV (the reverse transcriptase inhibitors ): Certain protease inhibitors can reduce the amount of virus in a person infected with HIV by as much as 99%.
But a protease inhibitor alone is not a cure for HIV infection or AIDS. The researchers studying these drugs still have a number of questions about how well they will work and how they should be used.
This section answers some of the basic questions about protease inhibitors. For the questions that can't be answered now, this page tries to give the best information available. This information will change as protease inhibitors are used by more people with HIV infection and as more is learned about how they work. So decisions about using protease inhibitors-in clinical trials and later when they are approved-should be made with the help of your physician and the team of healthcare workers involved in the clinical trials.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
1. What are HIV infection and AIDS?
One of HIV's favorite targets is a white blood cell called a T helper cell or CD4 cells. These blood cells are important because they tell other infection-fighting cells when to start working. HIV destroys CD4 cells, and when the number of CD4 cells drops to a certain level because of ongoing HIV infection, the body's immune system weakens. As a result, organisms such as fungi, viruses, and parasites that can live inside most people without causing disease can cause serious infections in people with HIV. When these infections occur, or when the number of CD4 cells drops below a certain level, a person with HIV infection is said to have AIDS.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
2. What is HIV protease?
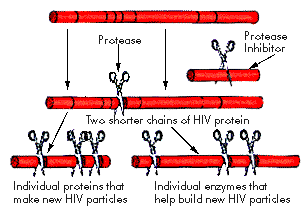
Figure 1:
HIV (the AIDS virus) can make new copies of
itself inside
an infected cell. One step in making these new copies is to cut long
chains of
proteins and
enzymes into shorter
chains. The "scissors" HIV uses to cut these chains is one of its
enzymes,
called protease. Protease inhibitors gum up the protease "scissors"
and stop
them from cutting. As a result, the new viruses produced can't infect
other
cells. (See Figure 2. (Illustrations by Neil
O.
Hardy)
Protease is one of HIV's enzymes, and it is required to continue the process of HIV infection. Its job comes near the end of the HIV replication process. By then, HIV has already entered the cell's nucleus and has made long chains of proteins and enzymes that will form many new copies of HIV. But before they can start working correctly, the long chains have to be cut into smaller pieces (Figure 1). The HIV protease enzyme is like a "chemical scissors" because it cuts the long chain into shorter pieces.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
3. What are protease inhibitors and how do they work?
New copies of HIV are still made and still push through the wall of the infected cell (Figure 2) even if the long chains aren't cut up into the correct smaller pieces. But these new copies of HIV are "defective" (not completely formed), so they can't go on to infect other cells.
Protease inhibitors can greatly reduce the number of new, infectious copies of HIV made inside cells. If protease inhibitors succeed in making most new HIV viruses defective, HIV infection would not spread inside the body as quickly as it does now.
Sometimes you will see the term proteinase inhibitor. It is the European name for protease inhibitor.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
4. Will protease inhibitors get rid of HIV?
Even so, if protease inhibitors do greatly slow the pace at which HIV makes new copies of itself, fewer new cells would be infected by HIV, and cells already infected will eventually die. As a result, because there is less virus, fewer CD4 cells would be infected, fewer would be destroyed, and an HIV- infected person could stay healthier longer. So controlling the amount of virus would help a person fight off other infections longer and continue to live an active life.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
5. How do protease inhibitors differ from other available anti-HIV drugs?
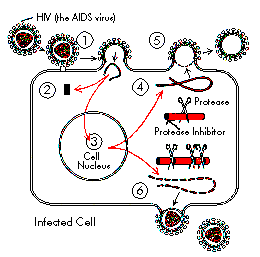 Figure 2:
Figure 2:
(1) HIV enters an uninfected cell.
(2) Reverse transcriptase inhibitors can stop duplication of HIV's genetic material.
(3) Without reverse transcriptase inhibitors, HIV's genetic material can get inside the cell's nucleus--its command center--where it makes long chains of proteins and enzymes.
(4) Protease inhibitors can stop the cutting of long chains of HIV proteins and enzymes into short chains.
(5) Protease inhibitors result in the formation of "empty" viruses that can't infect new cells.
(6) Without protease inhibitors, short chains of HIV proteins and enzymes make new viruses that can infect other cells.
This step in the HIV replication process happens soon after HIV infects a cell--much earlier than the step in which protease inhibitors are involved (Figure 2). Because protease inhibitors and reverse transcriptase inhibitors work at two separate steps in the HIV replication process, most HIV experts believe that the best way to give a protease inhibitor is to combine it with at least one or, if possible, two reverse transcriptase inhibitors. If a person has been taking one or two reverse transcriptase inhibitors for a long time and is not doing well, a protease inhibitor should be started with one or two different reverse transcriptase inhibitors.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
6. What protease inhibitors are being studied now?
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
7. Can protease inhibitors be combined with other drugs?
Protease inhibitors in the final stages of
development
(as of 7/31/96)
Drug name(s)* Maker Stage of development Invirase Hoffman-La Roche Approved for use in combination (saquinavir, RO-31-8959) with reverse transcriptase inhibitors (AZT, ddl, ddC, d4T, 3TC) Norvir (ritonavir, Abbott Approved for use in combination ABT-538) with reverse transcriptase inhibitors Crixivan (indinavir, Merck Approved for use in combination MK-639) with reverse transcriptase inhibitors Viracept (nelfinavir, Agouron In final trials in people with HIV infection AG-1343) *The first drug name in each group, spelled with a capital letter, is the brand name--the official name a drug gets when it is approved by the FDA, or is close to being approved. The second name in each group, spelled without a capital letter, is the generic name--the one that is usually used during later trials of a drug. The third name, which always has a number in it, is the name a company uses when it first starts to test a drug. With reverse transcriptase inhibitors, the drug names most often used--AZT, ddl, ddC, d4T, and 3TC--are abbreviations of the chemical names of the drugs.
Protease inhibitors in the early stages of development
(as of
7/31/96)
Drug name(s)* Maker Stage of development VX-478, 141W94 Glaxo-Wellcome/ In early trials in people Vertex with HIV infection KNI-272 (dynostatin) Nikko Kyoto In early trials in people Pharmaceutical and with HIV infection National Cancer Institute U-103373 Upjohn In early trials in people with HIV infection CGP-53437 Ciba-Ceigy In laboratory tests Hoe/Bay-793 Hoechst-Bayer In laboratory tests SR-41476 Sanofi In laboratory tests Other companies, including Boehringer Ingelheim, Bristol-Myers, Squibb, Lilly, Parke-Davis, Sandoz, Searle, and SmithKline Beecham, have been working on protease inhibitors. *See footnote to the first table for an explanation of the different types of drug names.
It is still too early to tell which combinations will work best. The best combination for one person may not be the best for another. Each combination involving protease inhibitors will have to be looked at carefully to make sure that the combination does not cause a lot of new side effects or increase the side effects of the other drugs. And it is important to remember that individuals will differ from others not only in how well a combination works for them, but also in what side effects may develop.
There is a simple explanation for why HIV drug experts don't expect bad interactions between protease inhibitors and the reverse transcriptase inhibitors like AZT: Protease inhibitors are processed by the liver, and drugs like AZT are processed inside nonliver cells and eliminated from the body through the kidneys. But other drugs used by people with HIV and AIDS are processed by the liver, just as protease inhibitors are. So the chance for interactions between those drugs and protease inhibitors is higher. People with HIV infection who are taking other drugs-especially antibiotics, anti-TB drugs, antihistamines (for allergies), antifungals, and antidepressants-should make sure their primary care physician reviews possible drug interactions when considering whether to start treatment with a protease inhibitor.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
8. Can protease inhibitors be combined with each other?
The first protease inhibitor combination being studied in people is ritonavir (Norvir) plus saquinavir (Invirase). There are two reasons why this combination is attractive: First, the chance for cross-resistance to the two drugs is low. (See 11 below.) Second, ritonavir slows the rate at which saquinavir leaves the body, so more saquinavir is around longer to attack the virus.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
9. What side effects do protease inhibitors have by themselves?
Some people have had a hard time with side effects like nausea and diarrhea when they start taking ritonavir (Norvir). It may be possible to avoid these side effects by gradually increasing the amount of the drug for the first two or three weeks and by adding reverse transcriptase inhibitors only at the end of that time. One dosing pattern that works for many people is 300 mg of ritonavir twice a day for two to three days, 400 mg twice a day for two to three days, 500 mg twice a day until side effects fade, than the full dose of 600 mg twice a day. It is important to be taking the full dose of ritonavir after three weeks.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
10. What is resistance and how big of a problem is it?
Resistance is a complicated problem. HIV drug experts are still trying to figure out exactly what it means for people who are taking drugs for HIV infection. Resistance to a drug may not necessarily mean that a person should stop taking that drug and will never be able to take it again.
Some studies of reverse transcriptase inhibitors show that certain patterns of resistance can be a plus instead of a minus. Also, all of the viruses in an infected person's body don't suddenly become resistant to a drug at the same time. So a drug can continue to be effective against the many nonresistant viruses still in the body. If a protease inhibitor is taken with other anti-HIV drugs-AZT and 3TC, for example-those other drugs might be able to attack the viruses that are resistant to the protease inhibitor. And the protease inhibitor could attack all the other viruses that are not resistant to it.
As with other drugs, each protease inhibitor differs in how quickly resistance to it develops. And everyone with HIV will differ in how quickly their HIV viruses will become resistant to different protease inhibitors. Resistance will develop more slowly in people with only a little virus in their body and with relatively high CD4 counts. In people with a lot of virus in their body, resistance will probably develop more quickly. Protease inhibitor experts agree that the best way to avoid or delay resistance to a protease inhibitor is to take the drug exactly as recommended by the drug manufacturer, to be especially careful not to skip taking the drug, and to take the protease inhibitor in combination with one or more reverse transcriptase inhibitors (AZT, ddI, ddC, d4T, and 3TC).
But the most important thing to remember about taking protease inhibitors is that, if you're already taking one or more reverse transcriptase inhibitors and not doing well, it's best to start taking a protease inhibitor with reverse transcriptase inhibitors that you have never taken before or at least have not taken in a long time.
Return to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
![]() Return to the What, How, and When
Menu
Return to the What, How, and When
Menu
11. What is cross-resistance?
AIDS experts agree that cross-resistance is a problem that must be studied closely. But most say it is too soon to understand the relationship between resistance to drugs and how best to treat HIV, because new findings are made every day. For example, researchers studying saquinavir say recent studies suggest that high-level cross-resistance will not be a problem in individuals first treated with this protease inhibitor. And other research shows that viruses that become resistant to several protease inhibitors are still susceptible (not resistant) to some of the newer protease inhibitors being developed.
At this point, most experts believe that people will be able to take certain protease inhibitors at the same time--or perhaps one after another with other anti-HIV drugs.
This information was generously provided by:
International Association of
Physicians in AIDS
Care ©1996
Go to the Protease Inhibitor
Menu
Go to the HIVpositive.us Main Menu
39